Guidelines for Audiologists Providing Informational and Adjustment Counseling to Families of Infants and Young Children With Hearing Loss Birth to 5 Years of Age
Guidelines
About This Document
This guidelines document is an official statement of the American Speech-Language-Hearing Association (ASHA). The ASHA Scope of Practice in Audiology states that the practice of audiology includes providing services to individuals across the entire age span from birth through adulthood. The Guidelines for the Audiologic Assessment of Children From Birth to 5 Years of Age fulfill the need for more specific procedures and protocols for serving young children with hearing loss across all settings. The guidelines within this document are intended to facilitate the critical role audiologists assume when providing family-focused counseling within the context of pediatric hearing health care service delivery.
It is recommended that individuals who practice independently in this area hold the Certificate of Clinical Competence in Audiology and hold a valid state license where required by law. Additionally, ASHA certified audiologists abide by the ASHA Code of Ethics, including Principle of Ethics II Rule B, which states “Individuals shall engage in only those aspects of the profession that are within their competence, considering their level of education, training, and experience.”
The Guidelines for Audiologists Providing Informational and Adjustment Counseling to Families of Infants and Young Children With Hearing Loss Birth to 5 Years of Age were developed by an ASHA working group and approved by the ASHA Board of Directors in February 2008. The members of the working group responsible for the development of these guidelines were Pam Mason (ex officio), Allan O. Diefendorf (chair), Judith S. Gravel, David M. Luterman, Noel D. Matkin, Amy McConkey Robbins, and Anne Marie Tharpe. Roberta Aungst, vice president for professional practice in audiology (2004–2006), and Gwendolyn Wilson, vice president for professional practice in audiology (2007–2009), served as the monitoring vice president.
Introduction
The American Speech-Language-Hearing Association (ASHA) documents entitled Guidelines for the Audiologic Assessment of Children From Birth to 5 Years of Age ( ASHA, 2004a) and Roles, Knowledge, and Skills: Audiologists Providing Clinical Services to Infants and Young Children Birth to 5 Years of Age ( ASHA, 2006) emphasize the complex and unique nature of providing audiologic services to infants and young children and their families. [1] These documents advocate a continuous process of family-focused service delivery, where audiologists are simultaneously engaged in
-
overseeing early identification (screening) programs ( Joint Committee on Infant Hearing [JCIH], 2007),
-
establishing an accurate diagnosis of hearing loss (ASHA, 2004a),
-
coordinating timely audiologic services (ASHA, 2006), and
-
providing effective family support and counseling.
The JCIH Year 2007 Position Statement: Principles and Guidelines for Early Hearing Detection and Intervention Programs ( JCIH, 2007), also policy of ASHA, advocates principles that provide guidance for effective early hearing loss detection and intervention (EHDI) programs. Furthermore, the principles underlying JCIH position statements have been advocated for more than 25 years ( JCIH, 1982, 1991, 1994, 2000) and are the bases for successful EHDI outcomes. Included in these principles are the following:
-
All infants should have access to hearing screening using a physiologic measure at no later than 1 month of age.
-
All infants who do not pass the initial hearing screening and any subsequent rescreening should have appropriate audiologic and medical evaluations to confirm the presence of hearing loss at no later than 3 months of age.
-
All infants with confirmed permanent hearing loss should receive early intervention services as soon as possible after diagnosis but no later than 6 months of age.
These benchmarks must be balanced with the reality that issues related to medically compromised/fragile infants, individual coping styles, family systems, and cultural differences may not always permit adherence to these guidelines ( Matkin, 1998). In addition, families with limited resources (e.g., family support, financial stability, spiritual beliefs, effective communication) will often experience challenges in moving through an EHDI system in a timely fashion. Yet, through effective counseling, support services, and sensitivity to the implications of those challenges on the parents and child, audiologists can facilitate families' abilities to adhere to a timely management plan.
This document is the third in a series of practice policy documents ( ASHA, 2004a, 2006). These guidelines are intended to provide audiologists with information about supporting and counseling families that facilitates successful outcomes for those families being served by EHDI programs. Furthermore, this document is based on the premise that families desire and require relevant information, support, and individualized recommendations throughout the screening, diagnostic, and intervention process ( Harrison & Roush, 2002).
Prior to the 1990s, infants with severe and profound hearing loss were identified at around 2 to 2½ years of age ( National Institutes of Health, 1993; U.S. Department of Health and Human Services, Public Health Service, 1990). For children with lesser degrees of bilateral and unilateral hearing loss, the age of identification was often as late as school entry. Furthermore, identification was typically initiated by parents concerned about their child's auditory responses, their lack of or delay in speech and language development, or their poor performance in school.
Early identification paradigms have changed considerably because of the recognized benefits of early detection of hearing loss within the first year of life (e.g., Kennedy et al., 2006; Moeller, 2000; Yoshinago-Itano, Sedey, Coulter, & Mehl, 1998). Remarkable improvements in communication and developmental outcomes can be largely attributed to advances in the technologies available for detecting and diagnosing hearing loss, as well as those used for intervention, including amplification incorporating sophisticated signal processing capabilities and cochlear implants. Consequently, parents are no longer likely to be initiating the identification process. Rather, almost 99% of birthing hospitals in the United States provide, either by state mandate or voluntarily, early detection of hearing loss through “universal” newborn hearing screening programs. In turn, audiologists are confirming the newborn hearing screening result often within the first few months of life, and thereafter providing support throughout the EHDI process.
Yet, prior to audiologic confirmation of permanent hearing loss and certainly thereafter, families in contemporary society readily access health information through a variety of sources, including the Internet. It is now frequently the case that audiologists no longer select the information to provide to families, but rather filter the vast amounts of information (both helpful and potentially detrimental) that families bring with them to clinical appointments. These changes in the timing of early screening for hearing loss, information access, and subsequent accelerated service provision require an expanded set of counseling skills by audiologists.
This context necessitates that family-focused information and emotional support counseling be infused into all interactions with families during the EHDI process and within every opportunity for pediatric audiologic practice thereafter. As such, family-focused counseling is not a separate service or event. In supplying information and support to families, audiologists recognize and respond to families' emotional needs following newborn hearing screening, at the time of the confirmation of the hearing loss, and throughout childhood.
The ultimate goal of these clinical interactions is to support the development of informed, independent, and empowered families. To achieve this outcome, audiologists judiciously provide information and guidance and, as needed, emotional support. To this end, parents' questions and comments guide the quantity of information needed, the level of detail provided, and the amount of emotional support required ( Luterman, 2006b).
As seen in Figure 1, audiologists initially provide substantial emotional support so that families can gain emotional strength. At the same time, audiologists are providing informational counseling so as to increase parental knowledge and competency as they grow to become strong advocates for their children.
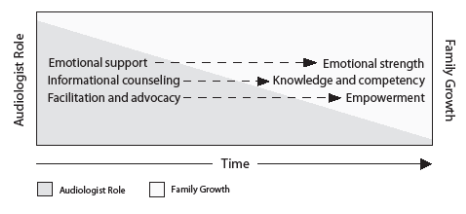
The roles of audiologists transition over time to those of facilitator and advocate. Audiologists strive to balance these roles while concurrently promoting family independence. Ultimately, the family becomes empowered to be the primary decision maker for their child.
Scope
The scope of this document is intended to facilitate family-focused counseling for parents and caregivers of children with hearing loss from birth to 5 years of age by audiologists as a routine and valued component of their clinical practice. Family-focused counseling provides emotional support to parents and caregivers as they adjust to the child's hearing loss, and informational counseling supports them as they learn about the myriad of audiologic, developmental, psychosocial, communication, and educational implications of permanent childhood hearing loss. It is important to note that counseling remains dynamic while it is infused into all aspects of service delivery, sometimes comprising information dissemination and exchange (content counseling), and sometimes involving the provision of emotional support. Throughout the child's formative years, counseling is an integral part of comprehensive service provision.
Terminology
Informational Counseling
Informational counseling is the imparting of information to families about a broad range of topics throughout childhood, including, but not limited to, the following:
-
audiogram interpretation
-
amplification/technology options
-
educational options
-
communication options
-
advocacy and public health and education policies
The audiologist's challenge is to provide sufficient information to assist families in decision making. Clear, concise explanations and information are needed. Terminology that misleads or confuses parents may influence a family's acceptance of hearing loss and postpone or at least delay the implementation of needed services. Additionally, audiologists are continually balancing education and guidance with their role as facilitator and advocate for informed decision making by families.
Adjustment to Hearing Loss Counseling
Given an appropriate support system, families can grow and change. Furthermore, families can and do directly influence their children's outcomes. Therefore, time and effort directed at the family during the EHDI process will likely result in family growth that can benefit the child over time ( DeConde Johnson, 1997). Adjustment to hearing loss counseling refers to the support provided by audiologists to families as they learn of their child's hearing loss and attempt to recognize, acknowledge, and understand the realities of having a child with hearing loss.
It is within the scope of practice in audiology to infuse emotional support during interactions with families ( ASHA, 2004b). Yet, audiologists must be vigilant in observing the few parents who demonstrate severe emotional responses to their child's diagnosis, particularly when those responses continue for lengthy periods of time and/or become more acute over time. In such cases, the parent's need for counseling or other supports may be beyond the scope of practice for audiologists, who should then be prepared to refer families to appropriate mental health care professionals.
Family Focused
Family-focused service provision attempts to achieve a balance between a systems- and technology-driven approach to EHDI. Although current public policy supported by scientific evidence endorses timely progression from identification of hearing loss to intervention ( JCIH, 2007), it is recognized that not all families can or will be able to comply with recommended benchmarks. Families do not process or accept new information with equal speed and accuracy. Therefore, regardless of the age of identification, the implementation of intervention services should progress at the family's desired pace. The desires and needs of the family must be acknowledged and supported, and given equally high priority as any public or institutional policy, keeping in mind that families are their children's primary decision makers and change agents. That is, throughout the diagnostic and early decision-making process and, later, as the individualized family service plan (IFSP) is developed, the family decides a course of action that best meets their family's needs at these critical points in time.
The impact on and/or influence of a family's cultural background also should be considered during assessment and intervention services provision. Potential linguistic and cultural barriers to interacting with families must be identified and a plan developed to address these needs. This helps to ensure effective communication and follow-up. Culturally and linguistically appropriate modes of communication, which may include the use of interpreters or translators, should be used during assessment and management ( Scott, 2002).
Families should be actively involved in the assessment and intervention process to the extent they desire and to the extent feasible given the complex nature of audiologic service delivery. The family's rights (including informed consent and confidentiality issues), reasonable expectations, reasonable needs, and preferences are paramount and must be considered throughout the provision of services. Additionally, EHDI systems must honor racial, ethnic, cultural, and socioeconomic diversity of families.
Unbiased Information
This document advocates the concept that families make informed choices for all aspects of their children's communication and educational development. Optimally, decision making is based on the best information that is available at the time, which the family receives through the audiologist as well as other sources. These decisions are made as families weigh the information they receive along with their desires for their child. Unbiased implies that only families are in the position to decide what outcomes they want for their children. Unbiased also implies that information provided to families is delivered in a straightforward manner without filters or hidden agendas. Providing unbiased information requires a recognition and revelation of one's own biases and opinions, fully disclosing any biases to families by stating the same, and then providing a basis for the opinion.
It is important to remember that the term unbiased does not imply that audiologists cannot or should not offer their expert opinions to families. Indeed, decisions families make are facilitated by the information provided by audiologists regarding, for example, the specifics of the child's hearing loss and amplification and communication options. This input is valued by and critical to families as they consider the myriad of choices and decisions that EHDI systems afford ( Harrison & Roush, 2002). Once families are ready to make informed decisions about desired outcomes, audiologists are then obligated to inform families on how best to achieve those outcomes.
Best practice is based on several premises that require audiologists to have firsthand, current knowledge of (a) published studies, including outcomes research and guidelines that support evidence-based practice; (b) children having a wide range of hearing loss (this implies that audiologists need to have a broad range of clinical experience); (c) auditory development and opportunities afforded by amplification and implantable devices technologies; (d) early intervention and educational practices and opportunities; and (e) public health and education law. All of these pieces of information are of great worth to families. It is the clinician's responsibility when counseling families to separate biased views from professional delivery of up-to-date information, and to ensure that families know the difference.
Family Stress
Depression is a common stress-related response for hearing parents of children with hearing loss. Evidence suggests that mothers are more inclined than fathers to experience depression in response to their child's hearing loss ( Mavrolas, 1990; Meadow-Orlans, 1995; Prior, Glazner, Sanson, & Debelle, 1988). Maternal depression places children with hearing loss at additional risk for emotional, communication, and cognitive difficulties, because of the implications for emotional availability and effective interactions between mothers and children ( Cohn, Campbell, Matias, & Hopkins, 1990; Field et al., 1988; Radke-Yarrow, 1998). Watson, Henggeler, and Whelan (1990) were able to show that a lack of social competence in hard of hearing youths occurred in correlation with parental stress experience. Increased behavioral problems were associated with poor emotional adaptation and a generally stressed family situation.
In a classic contribution to the field, Green and Solnit (1964) recognized more than 40 years ago that some parents with children having chronic conditions have a tendency to overprotect and overindulge their children, leading to overly dependent children and compromised developmental progress. For example, parents may harbor long-term fears that their “vulnerable child” ( Green & Solnit, 1964) will experience “changes” in hearing over time.
Grieving also may be a common response of parents who have just learned about their child's hearing loss. Parental grieving may occur at various times in the EHDI process, during the early school-age years, and throughout the active years of parenting. That is, grief is a complex and evolving emotional response that is internalized differently and triggered differently at various times throughout the time span of parenting a child with hearing loss. Additionally, grieving will not occur in an orderly manner or have a finite endpoint. As such, it is more realistic to consider various emotions as reflecting different states rather than different stages of grief. Often in a Western culture our manner of rational thinking is linear, yet the grief and healing process may be better considered as it is in Native American cultures. That is, grieving and healing can best be illustrated not as a straight ascending line but as a circular, yet upward, spiral (see Figure 2).
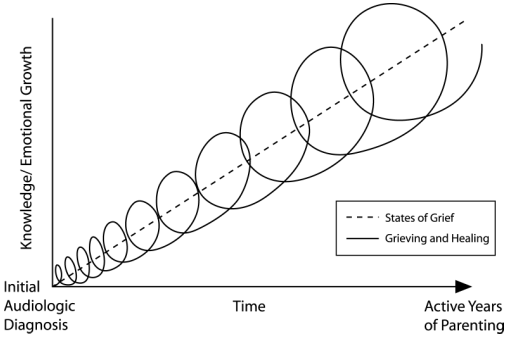
Although families learn to cope with adversity over time, they still revisit old concerns and experience old feelings, but often with better developed coping skills and with greater cognitive awareness. In other words, grief is chronic and continues to be triggered by unexpected events and at different times.
Applying Information and Adjustment Counseling to the EHDI Process
The following sections reflect stages in the EHDI process that are considered to be critical in the transition of families as they integrate children into their family structure and culture. In turn, the following sections of this guidelines document propose recommendations for best practices for counseling families made on the basis of best data available, while recognizing that evidence for any specific counseling approach is currently limited.
I. Newborn Hearing Screening
A. Informational Counseling
Audiologists are involved with all aspects of early identification of hearing loss, including program development, staff training, coordination, management, assessment of program quality, oversight of outpatient referral, and reducing lost to follow-up ( JCIH, 2007). Audiologists are the most qualified professionals to provide ongoing training and oversight of hospital nursery staff relative to the newborn hearing screening process ( JCIH, 2007). As such, and to the extent possible, audiologists should be the professionals who communicate with parents when a baby has not passed a hearing screening. However, it is recognized that within certain medical settings audiologists may not be available to convey the results before hospital discharge. Under those circumstances, audiologists ensure that others (such as nurses, technicians, or physicians) provide screening outcomes in oral and written forms and in a sensitive and considerate manner.
To facilitate this process, in-service education should always include information about how hearing screening results are presented to families, assuring that parents understand the reasons that a failure might occur in the nursery, appreciate the need to promptly follow-up with further screening or audiologic testing, and that early hearing loss detection often occurs over multiple clinical visits.
The following principles support effective informational counseling:
-
Communication with parents is confidential and presented in a family-focused manner.
-
Information is delivered in a clear and concise manner avoiding technical jargon.
-
Parents are given the opportunity and encouragement to ask questions.
Initial information in verbal and written forms and in the language used by families in the home should include
-
the rationale for screening of the newborn for hearing loss,
-
a description of screening procedure(s) and possible outcomes,
-
explanations for a failed screening outcome and its implications,
-
the importance of prompt follow up ( ASHA, 1996, 2004a; JCIH, 2007),
-
reasons why additional testing might be needed.
It is important to remember that if information about the screening process is provided only after a mother is admitted to the hospital to deliver her child, she may not have the level of concentration needed to consider adequately the information being presented. Therefore, it is recommended that educational materials also be
-
provided as part of hospital prenatal education programs and/or public health clinic outreach programs,
-
written at a 4th to 5th grade literacy level,
-
available in the preferred language of the family.
As already noted, recommendations for follow-up audiologic services (i.e., second stage outpatient rescreen and/or direct referral for testing by an audiologist) should be delivered in person to the parents by the audiologist. Use of the phrase “referral for further testing” rather than the term “failure” is more sensitive language and less alarming for conveying screening results and recommendations. Presenting these findings in a positive manner that emphasizes their importance may help to ensure that recommendations for additional testing are followed. Because of mitigating circumstances, communicating this information to parents of children in the well-baby nursery may be different than communicating the same results to parents of children who have extended stays in the NICU. If follow-up is needed, families should receive
-
explicit recommendations on how to secure follow-up testing, including names and phone numbers of follow-up screening facilities;
-
an audiologist to whom to direct questions in the interim;
-
local, state, and national resources to obtain information regarding subsequent stages of the EHDI process.
Additionally, although the goal of universal newborn hearing screening is to identify all infants with developmentally significant hearing loss, it is recognized that some children with minimal to mild degrees of hearing loss and unusual configurations of hearing loss will pass the newborn hearing screening ( Johnson et al., 2005). Similarly, children who experience late-onset hearing loss ( Fortnum, 2003) also are likely to pass newborn screening ( JCIH, 2007). When children have passed a newborn screening and at a later date are diagnosed with permanent types of hearing loss, this may complicate acceptance of the diagnosis by some families. Therefore, despite passing a newborn hearing screening or when families choose to not participate in screening, parents should be counseled about the need for ongoing surveillance and periodic monitoring of auditory and speech-language skills throughout early childhood ( JCIH, 2000, 2007).
B. Adjustment Counseling
Despite advances in screening technology and undeniable advantages of early intervention for hearing loss, there are emotional challenges associated with the newborn screening process for families ( Tharpe & Clayton, 1997). Consider that because of the advent of universal newborn hearing screening, parents are receiving unsolicited information about the program and their infant's hearing screening outcome at a sensitive and potentially vulnerable time. Consistent with informed consent and ethical practice, parents should be informed through verbal and written information that their newborn's hearing will be screened prior to hospital discharge, and screening outcomes also must be communicated. Parents should have the opportunity to opt out of the hearing screening for personal or religious reasons. Regardless, it is important to provide support counseling at this sensitive and emotionally fragile stage of the EHDI process. Adjustment counseling for families whose infants have failed a screening may include listening and responding to fears or concerns expressed by families, and ensuring follow-up of the failed screening in a timely manner to ameliorate stress and anxiety in families.
The timing of receipt of screening results coupled with the manner in which this information is conveyed has the potential to interfere with parent-child bonding, which is essential to the mental health of children ( Gregory, 1999, 2001). Therefore, this is a critical juncture in the identification process and might well determine whether parents comply with the recommendation for further assessment.
There might be occasional circumstances when hearing screening at a later time would be more appropriate for some families ( Eichwald, 2007; Luterman, 2007; Young & Tattersall, 2007). A small percentage of parents may refuse the in-hospital hearing screening, and, particularly in cases of the medically fragile NICU infants, families may choose to defer hearing screening. Under these circumstances, information about hearing screening, hearing loss, developmental milestones, and the availability of hearing screening after hospital discharge should be provided. Families should be supported in whatever decision they make regarding the screening process. However, families also should be made aware that in some states data on babies missed and/or those who refuse the hospital-based newborn hearing screening are reported to the state ( National Center for Hearing Assessment and Management, 2007).
Despite these challenges, there is evidence that the majority of parents of children with normal hearing and hearing loss desire newborn hearing screening and recognize the importance of early detection of hearing loss even when parents experience stress and anxiety at the time of diagnosis ( Barringer, Mauk, Jensen, & Woods-Kershner, 1997; Davis et al., 2006; Luterman & Kurtzer-White, 1999; Watkin, Beckman, & Baldwin, 1995). Therefore, the importance of coupling the screening process with parent information and support is crucial for facilitating smooth and timely transitions to the diagnostic process. Personnel involved in screening programs should be vigilant about improving outcomes (decreasing both the false positive and false negative rates), enhancing the manner and content of information provided to families, and optimizing the timing, delivery, and quality of information from the newborn hearing screening ( Arnold et al., 2006; Davis et al., 2006).
II. Confirmation of Hearing Loss
A. Informational Counseling
An audiologist is typically the first and most desired professional who bears the responsibility for describing the hearing loss and its implications to family members ( Harrison & Roush, 2002; Luterman & Kurtzer-White, 1999). This responsibility requires audiologists to be knowledgeable, skilled, and experienced in providing information that might be upsetting, stress-evoking, and even painful for some families. Equally important is the follow-up emotional support, guidance, and education that must be provided to families ( Matkin, 1988). It is important to remember that it is at this point in service delivery where individualized continuity of care by an audiologist is initiated.
In the initial stages of diagnosis and confirmation of hearing loss, the audiologist will need to assume a substantial role in providing information and explaining procedures for assessing hearing in children. This may include the following:
-
reasons why sleeping during testing is desirable for some tests, but not others;
-
reasons for the use of moderate sedation to achieve optimal test conditions and why medical monitoring of the child's health status is required;
-
explanations of different test procedures and why each is important;
-
explanations for why some tests may need to be repeated periodically.
Sharing audiometric results is a routine matter to audiologists, and frequently the initial interactions with families take on the effect of a rehearsed verbal template, in which the details of complex tests are explained in lay terminology. Although a necessary component of the counseling process, this imparting of test results, or informational counseling, can be perceived by the listener as a way of maintaining an uncaring professional distance. Beazely and Moore (1995) have discussed this in terms of “wearing an expert mantle” rather than making genuine, heartfelt contact. It is recommended that initially, audiometric results be explained to families in functional terms. In other words, families need to understand the impact of the hearing loss on a child's development more than the axes on the audiogram and hearing levels in decibels.
Because 90% or more of infants with hearing loss are born to hearing parents, most families have very little knowledge of childhood hearing loss. Furthermore, some parents may still be integrating their baby into the family unit with natural uncertainty and insecurity. Yet, families do possess parental instincts and a developing knowledge of their child and should be enlisted as collaborators in all aspects of the diagnostic process rather than being treated as passive participants. It is well established that involvement of families in the provision of clinical services is crucial for families' acceptance of hearing loss ( Luterman, 1999). Collaboration may include active roles such as
-
shaping the priorities and objectives of the visit;
-
providing descriptions of their child's auditory behaviors, either through conversation or completion of questionnaires;
-
sharing observations of their child's development and behavior;
-
participating with the child in demonstration of skills or compliance with the test battery;
-
providing feedback on the child's behavior throughout the behavioral audiologic test battery (i.e., how representative was the behavior of the child?).
A family's presence and/or participation allows the audiologist to explain the purpose of each step of the assessment, which in turn improves the family's ability to understand the findings of an otherwise abstract and technical test process.
It is recommended that during the confirmation of hearing loss
-
follow-up testing to confirm the initial diagnostic impression be scheduled as soon as possible to minimize the family's concern during the diagnostic phase; when possible, audiologists contact families ahead of time to explain the upcoming tests;
-
all diagnostic testing be conducted by the same audiologist in order to enhance continuity of care, encourage the development of rapport and trust, and minimize the likelihood of receiving different interpretations of the results from different audiologists;
-
parents' questions and comments guide the quantity of information and the level of detail provided;
-
audiologists provide time for parents to discuss their problems and concerns.
B. Adjustment to Hearing Loss Counseling
Audiologists should be aware that first impressions may set the tone for subsequent interactions with families. Therefore, a positive and respectful attitude is a necessary first step for developing an effective rapport with families. Respect includes sensitivity to nontraditional family structures, socioeconomic circumstances, cultural diversity, and differing viewpoints, regardless of whether those views are mutually embraced or whether realities are completely understood. Once rapport and respect are established, a sense of trust can evolve, which is strengthened as the relationship continues. The audiologist allows for the time necessary to establish such trusting relationships, even at the risk of creating slight delays in the diagnostic process.
Adjustment to hearing loss counseling by audiologists at this important juncture may include the following:
-
recognizing a family's fragility during the EHDI process;
-
recognizing the impact of the diagnosis of hearing loss on a family, including the child's siblings, grandparents, and other extended family members;
-
identifying family supports (e.g., friends, clergy) and encouraging families to seek their assistance when needed;
-
focusing on the family's strengths and special needs within the context of their cultural and value systems;
-
recognizing the difference between acute grief and clinical depression, and making appropriate referrals;
-
providing emotional support.
For counseling to be most effective, informational and adjustment counseling must be balanced. Although families will need information to facilitate decision making, many times families are not requesting information, but rather are expressing an emotional or affective concern about their child's recently identified hearing loss. That is, many times a family's message or questions will contain both content and affective components, and deciding which component requires priority is critical in developing a trusting relationship. The ability to distinguish content from affective components is referred to as “differentiation” ( Cormier & Hackney, 1999). It is one of the primary learning objectives in counselor education and is essential in the developing relationship between audiologists and families. Cormier and Hackney advocated that audiologists' responses should reflect the patient's or families' intent. That is, when a family requests information, the audiologist should respond with information, and when a family expresses an emotion, the audiologist should let the family know that the emotion was acknowledged and respected.
By having their emotional needs addressed, families may be more amenable to new information and more likely to make informed decisions. Yet, some audiologists may feel compelled to protect families from emotional reactions after receiving unexpected, upsetting, and potentially stress-evoking information ( Luterman, 2001). Any effort to rescue families (i.e., to imply the audiologist's approach guarantees a positive outcome) should be avoided, as this may actually foster dependency. Families need to progress at their own rates through various stages of personal adjustment.
An awareness of the stages of grief as a response to hearing loss is not sufficient for understanding a family's reaction to the confirmation of hearing loss. That is, Luterman (2006a) noted that the grief reaction of parents to the identification of hearing loss is not similar to the loss of a loved one to death. In death, there is finality to the grief; there is a burial and life can go on, albeit with pain and loss. With hearing loss, grief can be chronic, lived every hour of every day. The child may be a constant reminder to the parents of this loss. No matter how well adjusted the parents seem to be to the reality that their child has a hearing loss, there can be trigger events (e.g., child's birthday party, anniversary of their original diagnostic evaluation, individualized education program [IEP] meetings) that remind them of the loss and those initial feelings of pain and sorrow may return.
In some cases, grief associated with the diagnosis of hearing loss in children may result in clinical depression in parents. It is important for audiologists to recognize the signs of clinical depression, as opposed to acute grief, to help identify which families would benefit from referral to a mental health professional. The clinical signs of depression include
-
not keeping appointments;
-
deep feelings of sadness;
-
difficulty thinking, concentrating, remembering, or making decisions;
-
feelings of hopelessness, pessimism;
-
loss of energy or increased fatigue;
-
insomnia;
-
withdrawal/isolation from family.
Providing emotional support to families involves different communication skills than informational counseling, including the ability to talk less, listen more, and listen actively ( English, Lucks, Rojeski, & Hornak, 1999). Clinicians need not be afraid of periods of silence, tears, or expressions of anger. Silence may be a time when parents are attempting to integrate and think about their feelings and it is important that parent silence not be interrupted. Audiologists need to be comfortable with the silence and allow families this time. Tears also are a natural expression of grief. The simple act of handing a tissue to a distressed parent is a silent form of acknowledgment and support of the parent's feelings.
In addition, anger is often a reflection of a family's fear, a sense of violation of expectation, and a loss of control. However, anger is not necessarily a judgment on the audiologist's competency. Provision of emotional support, despite this anger, is crucial. Audiologists must be especially sensitive to families whose vulnerability and fragility (e.g., due to extended time in NICU, chronic illness, limited parental education, concurrent family stressors) necessitates extra time for them to understand and accept their child's hearing loss. Recognizing a family's fragility assists in determining the rate that they can integrate and process information. This recognition can help audiologists respond sensitively and without defensiveness should they become the target of a family's anger or frustration.
Although the confirmation of hearing loss may evoke an emotional response, the audiologist should view this response as a revealing affective component in the evolving counseling process. The establishment of a positive professional relationship can bring comfort to families during this stressful time. Audiologists also should recognize that the magnitude of the hearing loss is not a predictor of the extent of the parental stress response. Regardless of the degree of hearing loss, it is the parent's perception of the problem that dictates the amount of support needed.
Lederberg and Golbach (2002) found a difference in the stress experience of parents with deaf and hard of hearing children at age 2 years but not at age 3. Early diagnosis and intervention appear to be the best prevention strategy against stress for the parents of deaf and hard of hearing children.
III. Intervention and Habilitation
A. Informational Counseling
Audiologists are responsible for providing families with unbiased information, recommendations, and appropriate educational and communication options based on family decisions and informed choices. As such, audiologists are responsible to families and not for families.
Children with hearing loss, even those with similar audiograms, represent a heterogeneous population. These children and their families will come to audiologists with a wide range of concerns. Listening to families about their hopes and desires for their children will guide this process. Informational counseling to families might include
-
communication options appropriate for the family's desire for spoken or visual language;
-
technology options, including candidacy for cochlear implants;
-
the range of educational options appropriate to their child's hearing loss and developmental needs, including encouraging families to observe intervention programs on-site;
-
provision of information relative to the importance of ongoing monitoring and verification of amplification;
-
hearing aid orientation, troubleshooting, and maintenance for families, other caregivers, speech-language pathologists, educators/early interventionists, and the child when appropriate;
-
long-term audiologic follow-up, including addressing questions of progressive hearing loss;
-
processes associated with educational transitions;
-
public law and advocacy relevant to public education and public access;
-
other informational resources including, but not limited to, Web sites, printed materials, and DVDs.
During this time, communication among the audiologist, the child's medical home ( American Academy of Pediatrics, 2005), and child's family is essential for securing appropriate services ( JCIH, 2007). This also might help avoid confusion from conflicting information or recommendations received from various allied professionals.
Audiologists should encourage parents to acknowledge and celebrate the capabilities, as well as the special needs, of their children. By the late preschool years, children should be included as much as possible in feedback and decision making in their own management. This will initially consist of small steps (e.g., selecting the color of their hearing aids, learning to check their hearing aid batteries) that can lead to enhanced self-esteem and greater independence.
An additional responsibility of audiologists is to advocate for the development of quality educational options within their communities. Currently, family decisions are too often based solely on availability of services; that is, selecting from a limited number of services rather than the selection of their most desired option for communication and education. Therefore, audiologists should advocate for the establishment of diagnostic teaching facilities and a range of educational options, if not available, within the community. In addition, it is important that audiologists participate on multidisciplinary management teams with emphasis on facilitating communication, social-emotional, and cognitive development and, later, academic performance. It also is important for audiologists to participate in the IFSP and, later, the IEP processes. As families increasingly become empowered to serve as effective advocates for their children (refer to Figure 1), the role of the audiologist as care coordinator should begin to shift to facilitator ( ASHA, 2006).
B. Adjustment to Hearing Loss Counseling
The infusion of counseling into all interactions with families, mentioned earlier in this document, is especially important at this juncture. With an expanding array of technologies, educational options, and communication modes, families are faced with making complex decisions very early in the intervention process. They will need information relative to a range of options provided in an unbiased, supportive manner.
Intervention should be provided with sensitivity to the family's readiness to proceed. There may be a wide time range of when families are ready to proceed with intervention. That is, some families come into the process with strong coping skills and extensive support structures allowing them to move forward in a timely manner.
Scorgie, Wilgosh, and McDonald (1998) summarized the most important variables for understanding the coping process under four headings:
-
family variables (e.g., family socioeconomic status, cohesion, hardiness, problem-solving skills/creativity, roles and responsibilities, and composition);
-
parent variables (e.g., quality of marital relationship, maternal locus of control, appraisal, and time/schedule concerns);
-
child variables (e.g., degree of disability, age, gender, and temperament);
-
external variables (e.g., stigmatizing social attitudes, social network supports, and collaboration with professionals).
Calderon and Greenberg (1993), as well as Calderon, Greenberg, and Kusche (1991), were able to show that successful coping on the mother's part has a significant influence on child development. The more successful the mothers were in acquiring helpful strategies for coping with their deaf child, the better developed the children's emotional sensitivity, reading competence, and problem-solving behavior. The children also exhibited less impulsive behavior, higher cognitive flexibility, and better social competence.
Webster-Stratton (1990) pointed out another crucial aspect of coping that demonstrates the close correlation between parental experience and parental behavior: Specifically, there was a close association between reported parental stress and more frequent use of punishment, discipline, and constraint in day-to-day parenting.
When families lack resources to engage in even the most basic aspects of service delivery, audiologists must consider the number and types of demands they make on families. Awareness of the challenges each family unit faces should guide the audiologist's expectations on the family's capacity to fully follow through with an early intervention plan. Thus, a lack of follow through with the audiologist's recommendations during this time may reflect a variety of underlying causes and should not be misconstrued as a lack of caring or, as is sometimes suggested, constituting child neglect.
Audiologists must balance their information counseling with families regarding the use of hearing technologies (e.g., digital hearing aids, cochlear implants, or FM systems), with the family's perceived enticement to technology as a “cure.” Although current technology has greatly ameliorated the impact of hearing loss, technology provision alone is not sufficient to the habilitation/intervention process. The temptation to consider technology (particularly cochlear implants) as a cure for deafness should be resisted, as this diminishes the challenges still ahead and ignores the need of families to spend time resolving their loss. At the same time, audiologists recognize when families are in need of information and support in exploring their options and opportunities for their children. Facilitating families' knowledge of options and opportunities sends a hopeful message of optimism and may prevent feelings of fear and isolation.
As intervention plans are initiated, it is important that both audiologists and families recognize that all decisions are subject to change over time. Although continuity of intervention is recognized as an important factor for successful outcomes, families should always be made aware that their initial choices are amendable.
Children might require a period of diagnostic teaching to inform this process. In a diagnostic teaching approach, appropriate individual goals are set, but the interventionist continually monitors the factors that are favorable or unfavorable to a child's learning. The focus of such an approach is prominently on the positive aspect of the question: “What are the techniques and supports that help this child learn most efficiently?” Diagnostic teaching allows for the determination of effectiveness of hearing technology options that may include hearing aids, cochlear implantation, and assistive devices. Moreover, the diagnostic teaching period allows for the determination of an effective method of communication and one preferred and used continually by all members of the family. Some families and children will best be served by auditory/oral approaches (speaking and listening) to communicate while others may require a system with visual supports. Diagnostic teaching also may reveal the presence of additional disabilities not previously identified ( Gallaudet Research Institute, Office of Demographic Studies, 2001).
A rich source of support for families may be found in their relationships with other families of children with hearing loss. Efforts should be made to provide families with formal and informal opportunities to meet and interact with other families with similar experiences when they desire such opportunities. Optimally, these are informed choices families make about when and which interactions would be most beneficial to them. Therefore, adjustment to hearing loss counseling in intervention and habilitation may include
-
provision of opportunities both formal and informal to meet and interact with other families of children with hearing loss. The type of interactions that individual families choose will be based on their need for information and their desires to learn more about one or more different communication and education options. These could include introductions to culturally Deaf, oral deaf, and hard of hearing adults who use different communication modes and technology;
-
opportunities to observe children and interact with young children who use various communication approaches and technologies;
-
development and facilitation of family support groups.
The audiologist's role in family support groups is one of facilitator, rather than instructor. Within family support groups, parents can validate each other's experiences in ways that audiologists cannot. This interaction also can lead to growing parental empowerment as information is shared among families. All family members, including grandparents and siblings, can benefit from attending such sessions or participating in support groups that focus on shared experiences of individuals with similar roles, rather than passively listening to information provided by professionals.
In supplying information to families, audiologists should recognize and respect the family's complex (and often recurring) feelings through the grieving process, not only at the time of initial diagnosis of hearing loss, but also at different intervention decision-making stages and transitions, and throughout the active years of parenting. That is, stress is a complex and evolving emotional response that is internalized differently and triggered differently at various times throughout the time span of parenting a child with hearing loss ( Luterman, 2006a).
Audiologists should be aware that families may be fearful that every subsequent audiologic assessment beyond the initial diagnosis has the potential of revealing additional difficulties or changes (decrements) in hearing threshold levels. Even families that have previously demonstrated excellent coping skills may need additional support upon learning that their child's hearing loss has progressed ( Brookhouser, Worthington, & Kelly, 1994). Furthermore, there is an important role for the audiologist in supporting families with the transition of their children from early intervention to preschool and through to the school-age years.
IV. Professional Preparation Concerns and Recommendations
Counseling in audiology has historically employed a medical model with an emphasis on providing content/informational counseling, and rarely providing emotional support. Additionally, over the past decade a medical model has served as the foundation for implementing a systems-driven paradigm (mandated universal newborn hearing screening) stressing diagnosis and intervention of hearing loss in the first 6 months of life, and providing parents and caregivers with information on the screening, follow-up, and intervention components of early detection.
Another change that has had an impact on service delivery is our nation's growing population diversity, requiring knowledge of and experience with multicultural counseling to respond to linguistic and cultural differences prevalent in the United States. As such, achieving benchmarks (i.e., positive language outcomes) in early detection is facilitated when family counseling and emotional support are actively infused into audiologic care within a systems-driven paradigm.
Professionals increasingly have become aware that family-focused counseling and instruction needs to be an integral component of screening, diagnosis, and intervention, employing the ongoing infusion concept already described. Because of the wide range of emotions associated with hearing loss, the need for formal and practical education in counseling seems apparent. Historically, preparation for addressing the emotional and personal needs of families has been limited ( Martin, Barr, & Bernstein, 1992; Martin, Krall, & O'Neal, 1989). However, the current Knowledge and Skills Acquisition Summary Form ( ASHA, 2003) provides a general acknowledgement of this need. More specific recommendations for the preparation of audiologists to provide counseling include the following:
-
Explicit coursework in curricula—expand traditional view of counseling to include dealing with emotional impact of diagnosis of childhood hearing loss on families:
-
knowledge of child development and necessary parenting skills as essential prerequisites to management;
-
knowledge of the grieving process and the role that emotional states play in the acceptance process;
-
knowledge of personal adjustment counseling;
-
knowledge of family systems theory;
-
knowledge of cultural differences;
-
knowledge of the impact of limited resources (e.g., financial, emotional) on a family's ability to cope with a stressor such as hearing loss.
-
-
Practical observation and supervised experience with
-
families with children of different ages in clinical and informal settings;
-
families in different stages of acceptance;
-
families at different points in the service delivery continuum;
-
family support groups;
-
mentor counselors.
-
Appropriate counseling is a critical variable in the habilitation/rehabilitation of individuals with hearing loss (see Crandell, 1997, and Luterman, 2001, for a review of these investigations). Yet, historically, little has been done to equip audiologists with these skills. McCarthy, Culpepper, and Lucks (1986) found that only 12% of university communication disorders programs in the United States offered coursework and practice in counseling. Almost 10 years later, the authors repeated their study and found essentially no change ( Culpepper, Mendel, & McCarthy, 1994).
Similarly, Crandell (1997) examined the availability of counseling instruction with audiology graduate programs. Results indicated that less than one half of the programs offered a counseling course. Moreover, only 27% of the audiology departments that offered a counseling course required that course to be taken. Because of this lack of required course work, programs estimated that only 18% of their students ever took a counseling course prior to graduation. With the recent transition of the entry level degree from a master's to a clinical doctorate plus additional required course work, this dearth in counseling education may be, at least, partially remediated. However, it will be important for professional organizations such as ASHA to monitor the provision of this course work as well as postprofessional preparation in this most critical requisite to quality audiology practices with the pediatric population.
V. Future Research Needs
Much remains to be learned about effective counseling approaches for use with families of children with hearing loss. Every effort should be made to enhance our knowledge base in this important area. Recommended research areas include the following:
-
psychosocial effects of newborn hearing screening on the child and the family
-
impact of false positive and false negative screening outcomes on families, including
-
stress factors
-
coping mechanisms
-
quality of life issues
-
-
parental understanding of content and retention of information relative to
-
all components of the in-hospital and outpatient screening process
-
a medical-based approach versus a family-centered approach and their integration
-
use of hearing aids, cochlear implants, and other assistive devices
-
speech and language development
-
-
parental compliance with follow-up relative to screening, assessment, and intervention:
-
method of communicating follow-up recommendations (written vs. oral)
-
impact of family's educational background and socioeconomic status
-
impact of family's cultural and linguistic differences
-
impact of NICU versus well-baby hospital stay on family's compliance with follow-up
-
-
key factors related to family satisfaction with services and transitioning from one to another, in particular
-
early intervention services
-
preschool programs
-
regular school system
-
-
factors that contribute to family fragility, such as
-
behavioral markers
-
family support systems
-
-
predictors for successful family outcomes
-
innovative approaches to the delivery of family counseling and support services for those who lack the resources that facilitate their ability to participate fully in the EHDI system
Our current body of counseling literature is largely based on late identification of hearing loss in children, not our current reality of early detection in the newborn period. As such, there is a great need for more current investigations into the counseling process and its effectiveness for families with newly identified infants with hearing loss. Such studies are recommended to test the validity of current counseling practices in early identification, diagnosis, and intervention. Additionally, much information may be gleaned from parent reports, questionnaires, and structured interview schedules that, when constructed in compliance with robust research principles, yield valuable first-person data that informs what clinicians may come to view as best practice.
VI. Summary
These guidelines were developed with the goal of infusing family-focused counseling within today's opportunities for early identification through a systems- and technology-driven model of service delivery (i.e., the 1–3–6 guidelines [ Centers for Disease Control and Prevention, 2006]). Within this framework, a family's individuality and resources, diversity, cultural background, coping style, and learning style are recognized, supported, and respected. These guidelines reinforce the goals of the Joint Committee on Infant Hearing and adherence to pediatric audiologic service delivery consistent with the 1–3–6 guidelines of EHDI ( Centers for Disease Control and Prevention, 2006; JCIH, 2007).
For counseling to be most effective, information counseling and adjustment counseling/emotional support must be balanced. The goal is to facilitate the development of informed, independent, and empowered families who will make good decisions for themselves and their child.
In some areas, there is a shortage of audiologists to comprehensively evaluate and appropriately manage infants and toddlers with hearing loss and counsel their families. As such, university education programs are encouraged to expand preservice curricula that address the unique knowledge and skills ( ASHA, 2006) needed for working with infants and young children with hearing loss in culturally sensitive and family-centered ways. In addition, in-service education and continuing education focusing on the infusion of counseling into all aspects of service delivery for infants and young children and their families also must be encouraged.
The foundation of outcomes studies upon which EHDI policies were implemented must be expanded. To the extent possible, counseling families during crucial periods of parenting should be evidence based and outcome directed.
References
American Academy of Pediatrics. (2005). Newborn and infant hearing screening activities. Available from www.medicalhomeinfo.org.
American Speech-Language-Hearing Association. (1996). Guidelines for audiologic screening [Guidelines]. Available from www.asha.org/policy.
American Speech-Language-Hearing Association. (2003). Knowledge and Skills Acquisition (KASA) Summary Form for certification in audiology. Available from www.asha.org/about/membership-certification/handbooks/kasa-tips.htm.
American Speech-Language-Hearing Association. (2004a). Guidelines for the audiologic assessment of children from birth to 5 years of age [Guidelines]. Available from www.asha.org/policy.
American Speech-Language-Hearing Association. (2004b). Scope of practice in audiology. Available from www.asha.org/policy.
American Speech-Language-Hearing Association. (2006). Roles, knowledge, and skills: Audiologists providing clinical services to infants and young children birth to 5 years of age [Knowledge and Skills]. Available from www.asha.org/policy.
Arnold, C. L., Davis, T. C., Frempong, J. O., Humiston, S. G., Bocchini, A., Kennen, E. M., & Lloyd-Puryear, M. (2006). Assessment of newborn screening parent education materials. Pediatrics, 117(5, Pt. 2), S320–S325.
Barringer, D. G., Mauk, G. W., Jensen, S., & Woods-Kershner, N. (1997). Survey of parents' perceptions regarding hospital-based newborn screening. Audiology Today, 9(1), 18–19.
Beazely, S., & Moore, M. (1995). Deaf children, their families, and professionals: Dismantling barriers. London: David Fulton.
Brookhouser, P., Worthington, D., & Kelly, W. (1994). Fluctuating and or progressive sensorineural hearing loss in children. Laryngoscope, 104, 958–964.
Calderon, R., & Greenberg, M. T. (1993). Considerations in adaptation of families with school-aged deaf children. In M. Marschark & M. D. Clark (Eds.), Psychological perspectives on deafness (pp. 27–47). Hillsdale, NJ: Erlbaum.
Calderon, R., Greenberg, M. T., & Kusche, C. (1991). The influence of family coping on the cognitive and social skills of deaf children. In D. Martin (Ed.), Advances in cognition, education and deafness (pp. 195–200). Washington, DC: Gallaudet University Press.
Centers for Disease Control and Prevention. (2006, October 27). National EHDI goals. Available from www.cdc.gov/ncbddd/ehdi/nationalgoals.htm.
Cohn, J., Campbell, S., Matias, R., & Hopkins, J. (1990). Face-to-face interactions of postpartum depressed and nondepressed mother-infant pairs at two months. Developmental Psychology, 26, 15–23.
Cormier, S., & Hackney, H. (1999). Counseling strategies and interventions (5th ed.). Boston: Allyn & Bacon.
Crandell, C. C. (1997). An update on counseling instruction with audiology programs. Journal of the Academy of Rehabilitative Audiology, 15, 77–86.
Culpepper, N. B., Mendel, L. L., & McCarthy, P. A. (1994). Counseling experiences and training offered by ESB-accredited programs: An update. Asha, 36(6), 55–58.
Davis, T. C., Humiston, S. G., Arnold, C. L., Bocchini, J. A., Bass, P. F., Kennen, E. M., et al. (2006). Recommendations for effective newborn screening communication: Results of focus groups with parents, providers and experts. Pediatrics, 117(5, Pt. 2), S326–S340.
DeConde Johnson, C. (1997). Understanding and advising parents and families. Hearing Review, 18–20.
Eichwald, J. (2007, July 17). Newborn hearing screening: A response to David Luterman. The ASHA Leader, 12(9), 24–25.
English, K., Lucks, L., Rojeski, T., & Hornak, J. (1999). Counseling in audiology, or learning to listen: Pre- and post-measures from an audiology counseling course. American Journal of Audiology, 8, 1–6.
Field, T., Healy, G., Goldstein, S., Perry, S., Bendell, D., Schanberg, S., et al. (1988). Infants of depressed mothers show depressed behavior even with nondepressed adults. Child Development, 59, 1569–1579.
Fortnum, H. M. (2003). Epidemiology of permanent childhood hearing impairment: Implications for neonatal hearing screening. Audiologic Medicine, 1(3), 155–164.
Gallaudet Research Institute, Office of Demographic Studies. (2001, January). Regional and national summary report of data from 1999–2000 Annual Survey of Deaf and Hard of Hearing Children & Youth. Washington, DC: Author. Available from http://gri.gallaudet.edu/Demographics/.
Green, M., & Solnit, A. J. (1964). Reactions to the threatened loss of a child: A vulnerable child syndrome. Pediatrics, 34, 58–66.
Gregory, S. (1999). Cochlear implantation and the under 2's: Psychological and social implications. Paper presented at the Nottingham Paediatric Implant Programme International Conference, Cochlear Implantation in the Under 2's; Research Into Clinical Practice, Nottingham, England.
Gregory, S. (2001, September). Consensus on auditory implants. Paper presented at the Ethical Aspects and Counseling Conference, Padova, Italy.
Harrison, M., & Roush, J. (2002). Information for families with young deaf and hard of hearing children: Reports from parents and pediatric audiologists. In R. C. Seewald & J. S. Gravel (Eds.), A sound foundation through early amplification (pp. 233–249). Warrenville, IL: Phonak AG.
Johnson, J. L., White, K. R., Widen, J. E., Gravel, J. S., James, M., Kennalley, T., et al. (2005). A multicenter evaluation of how many infants with permanent hearing loss pass a two-stage otoacoustic emissions/automated auditory brainstem response newborn hearing screening protocol. Pediatrics, 116, 663–672.
Joint Committee on Infant Hearing. (1982, December). Joint Committee on Infant Hearing 1982 position statement. Asha, 24(12), 1017–1018. Available from www.jcih.org.
Joint Committee on Infant Hearing. (1991). Joint Committee on Infant Hearing 1990 position statement. Asha, 33(3), 3–6. Available from www.jcih.org.
Joint Committee on Infant Hearing. (1994). Joint Committee on Infant Hearing: 1994 position statement. Asha, 36(12), 38–41. Available from www.jcih.org.
Joint Committee on Infant Hearing. (2000). Year 2000 Position Statement: Principles and guidelines for early hearing detection and intervention programs. American Journal of Audiology, 9, 9–29. Available from www.jcih.org.
Joint Committee on Infant Hearing. (2007). Year 2007 position statement: Principles and guidelines for early hearing detection and intervention programs. Pediatrics, 120, 898–921. Available from www.asha.org/policy.
Kennedy, M. B., McCann, D. C., Campbell, M. J., Law, C. M., Mellee, M., Petrou, S., et al. (2006). Language ability after early detection of permanent childhood hearing impairment. New England Journal of Medicine, 354, 2131–2141.
Lederberg, A., & Golbach, T. (2002). Parenting stress and social support in hearing mothers of deaf and hearing children: A longitudinal study. Journal of Deaf Studies and Deaf Education, 7, 330–345.
Luterman, D. (1999). The young deaf child. Baltimore: York Press.
Luterman, D. M. (2001). Counseling persons with communication disorders and their families (4th ed.). Austin, TX: Pro-Ed.
Luterman, D. (2006a). Children with hearing loss: A family guide. Hearing Review, 13(11), 18–24.
Luterman, D. (2006b, March 21). The counseling relationship. The ASHA Leader, 11(4), 8–9. Available from http://dx.doi.org/doi:10.1044/leader.FTR3.11042006.8.
Luterman, D. (2007, May 8). Technology and early childhood deafness. The ASHA Leader, 12(6), 43. Available from https://doi.org/10.1044/leader.FMP.12062007.43.
Luterman, D., & Kurtzer-White, E. (1999). Identifying hearing loss: Parents' needs. American Journal of Audiology, 8, 13–18.
Martin, F. N., Barr, M. M., & Bernstein, M. (1992). Professional attitudes regarding counseling of hearing-impaired adults. American Journal of Otology, 13, 279–287.
Martin, F. N., Krall, L., & O'Neal, J. (1989). The diagnosis of acquired hearing loss: Patient reactions. Asha, 31(11), 47–50.
Matkin, N. (1988). Key considerations in counseling parents of hearing-impaired children. Seminars in Speech and Language, 9(3), 209–222.
Matkin, N. (1998). The challenge of providing family-centered services. In F. Bess (Ed.), Children with hearing impairment: Contemporary trends (pp. 299–304). Nashville, TN: Vanderbilt Bill Wilkerson Center Press.
Mavrolas, C. (1990). Attachment behavior of hearing-impaired infants and their hearing mothers: Maternal and infant contributions. Unpublished doctoral dissertation, Northwestern University, Evanston, IL
McCarthy, P., Culpepper, N. B., & Lucks, L. (1986). Variability in counseling experiences and training among ESB-accredited programs. Asha, 28(9), 49–52.
Meadow-Orlans, K. (1995). Sources of stress for mothers and fathers of deaf and hard of hearing infants. American Annals of the Deaf, 140, 352–357.
Moeller, M. P. (2000). Early intervention and language development in children who are deaf and hard of hearing Pediatrics, 106 (3), E43 Retrieved from www.pediatrics.org/cgi/content/full/106/3/e43.
National Center for Hearing Assessment and Management. (2007). EHDI legislation. Available from www.infanthearing.org/legislative/index.html.
National Institutes of Health. (1993). Early identification of hearing impairment in infants and young children. NIH Consensus Development Conference Statement Retrieved from http://consensus.nih.gov/1993/1993HearingInfantsChildren092html.htm.
Prior, M., Glazner, J., Sanson, A., & Debelle, G. (1988). Research note: Temperament and behavioral adjustment in hearing impaired children. Journal of Child Psychology and Psychiatry, 29, 209–216.
Radke-Yarrow, M. (1998). Children of depressed mothers: From early childhood to maturity. New York: Cambridge University Press.
Scorgie, K., Wilgosh, L., & McDonald, L. (1998). Stress and coping in families of children with disabilities: An examination of recent literature. Developmental Disabilities Bulletin, 26, 22–42.
Scott, D. M. (2002). Multicultural aspects of hearing disorders and audiology. In D. E. Battle (Ed.), Communication disorders in multicultural populations (pp. 335–360). Woburn, MA: Butterworth-Heinemann.
Tharpe, A. M., & Clayton, E. W. (1997). Newborn hearing screening: Issues in legal liability and quality assurance. American Journal of Audiology, 6(2), 5–12.
U.S. Department of Health and Human Services, Public Health Service. (1990). Healthy People 2000: National health promotion and disease prevention objectives for the nation (DHHS Publication No. [PHS] 91-50212). Washington, DC: U.S. Government Printing Office.
Watkin, P. M., Beckman, A., & Baldwin, M. (1995). The views of parents of hearing impaired children on the need for neonatal screening. British Journal of Audiology, 29, 259–262.
Watson, S. M., Henggeler, S. W., & Whelan, J. P. (1990). Family functioning and the social adaptation of hearing-impaired youths. Journal of Abnormal Child Psychology, 18, 143–163.
Webster-Stratton, C. (1990). Stress: A potential disrupter of parent perceptions and family interactions. Journal of Clinical Child Psychology, 19, 302–312.
Yoshinaga-Itano, C., Sedey, A. L., Coulter, D. K., & Mehl, A. L. (1998). Language of early- and later-identified children with hearing loss. Pediatrics, 102, 1161–1171.
Young, A., & Tattersall, H. (2007). Universal newborn hearing screening and early identification of deafness: Parents' responses to knowing early and their expectations of child communication development. Journal of Deaf Studies and Deaf Education, 12(2), 209–220.
Notes
[1] The term family includes biologic and/or adoptive parents, foster parents, grandparents, or others who live with the child in a familial environment. Legal definitions of family may vary by jurisdiction. The title parents means the caregivers who share primary responsibilities for the child's care and welfare. Audiologists must honor all family relationships and maintain compliance with HIPAA regulations and other privacy requirements.
Index terms: children, newborns, infants and todders, early intervention, hearing loss, patient/family education
Reference this material as: American Speech-Language-Hearing Association. (2008). Guidelines for audiologists providing informational and adjustment counseling to families of infants and young children with hearing loss birth to 5 years of age [Guidelines]. Available from www.asha.org/policy.
© Copyright 2008 American Speech-Language-Hearing Association. All rights reserved.
Disclaimer: The American Speech-Language-Hearing Association disclaims any liability to any party for the accuracy, completeness, or availability of these documents, or for any damages arising out of the use of the documents and any information they contain.
doi:10.1044/policy.GL2008-00289










