Step 4: Make Your Clinical Decision
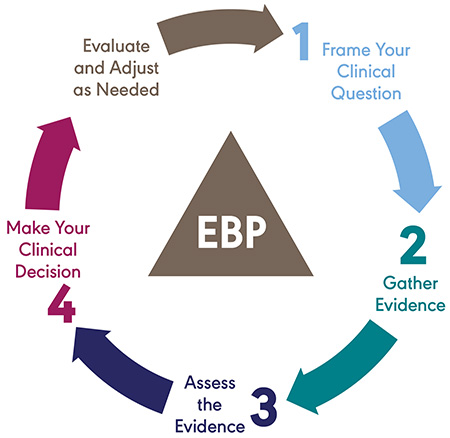
- Evidence-Based Practice
- Step 1: Frame Your Clinical Question
- Step 2: Gather Evidence
- Step 3: Assess the Evidence
- Step 4: Make Your Clinical Decision
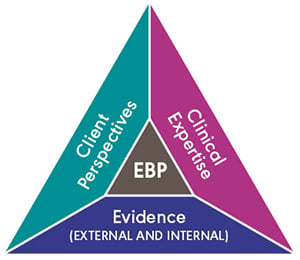
The final step of the EBP process requires you to make a clinical decision. To make an evidence-based decision, clinicians must consider evidence (both internal and external), assess the appropriateness of their clinical experience for the situation, and review the individual client’s perspectives and priorities—the three components of EBP.
Although this complex and nuanced process may seem difficult, the D.E.C.I.D.E. framework can help you easily remember and implement all four steps of the EBP process and can help guide you to a clinical decision.
Define
Define your clinical question, gather external and internal evidence, and determine the validity and trustworthiness of the results. You should complete the first three steps of EBP prior to making any clinical decisions. If you have not yet completed the previous steps of EBP, see the following:
Extrapolate
Extrapolate clinically applicable information from the external evidence. Although some results may directly align with your client and setting, often, you will need to determine whether the overall results are compelling and meaningful enough to apply to your clinical situation. Sometimes, there is simply a lack of external evidence about your clinical question. If there’s little or no external scientific evidence, then your treatment isn’t necessarily disqualified—it just requires careful consideration and monitoring.
Quick Tip:
A lack of evidence does not equate to evidence of no effect.
Consider
Consider your clinical expertise and the expertise of others. Use your training, knowledge, and clinical experience to collect and analyze internal evidence and to interpret and apply external evidence when making a clinical decision. Refer to the Audiology and Speech-Language Pathology scopes of practice and ASHA’s Code of Ethics, as needed.
Incorporate
Incorporate the needs and perspectives of your client, their caregiver, and/or their family into your assessment and intervention decisions. These needs and perspectives can provide insight into their priorities, values, and expectations. A client’s cultural or linguistic characteristics (e.g., status as an English language learner) can also impact how you interpret the internal evidence and how you apply the external evidence to your clinical decision. Understanding what is important to your client—and considering their unique characteristics when making a clinical decision—can help you develop your treatment plan, increase your client’s participation and engagement, and ensure that their goals are meaningful—not only clinically but also personally.
Develop
Develop an assessment or treatment plan by bringing together the three components of EBP. In some clinical situations, you may need to prioritize one of the EBP components (e.g., external scientific evidence reporting harm or a client’s preference/refusal); however, you should consider all three components.
- Use your clinical expertise to determine how to implement the external and internal evidence into your assessment or intervention sessions (e.g., adapting an evidence-based treatment into an engaging and individualized activity).
- Prioritize your client's perspectives to make the sessions meaningful. Include goals that are measurable and functional.
- Consider organizational or other barriers when developing your plan (e.g., access to materials, department protocols, transportation, or feasibility of implementation).
Quick Tip:
Be transparent with your client about the treatment plan, rationale, benefits, and potential harms.
Evaluate
Evaluate your clinical decision. Use a trial period, collect internal evidence, and analyze all of the clinical information to (a) ensure that the intervention is appropriate or (b) adjust your treatment plan as needed. EBP is a dynamic process and requires ongoing evaluation. If you don’t see progress, if your client’s needs or circumstances have changed, or if you need to re-prioritize the goals, you should cycle through the EBP process again to find another option that can better serve your client.